
News Release
MediQuant Honored with 12th Consecutive Weatherhead 100 Award
Read Now >



New Podcast
Exploring Healthcare’s Data and AI Landscape with MediQuant CEO Jim Jacobs
Listen Now >
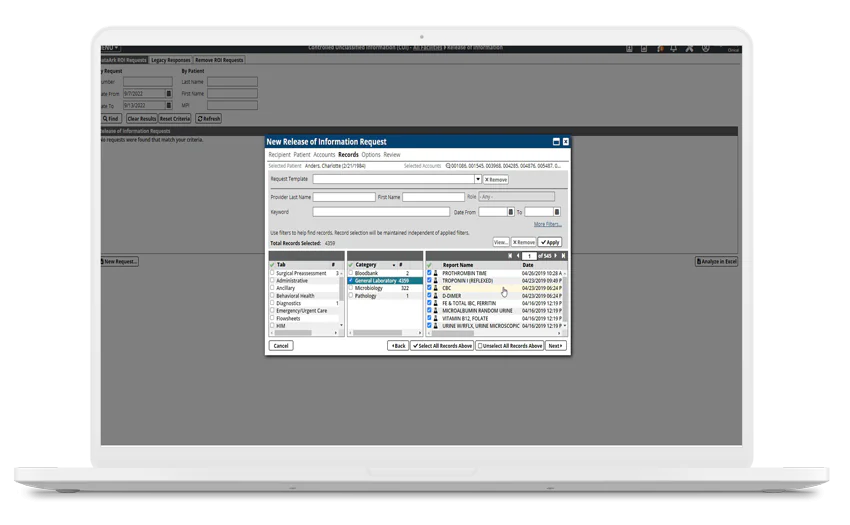

MediQuant is Healthcare’s Leading Enterprise Active Archive Platform
By partnering with MediQuant, you can reduce your IT footprint, create a positive user experience, and deliver high value data that is structured, secure, compliant and usable.
We accomplish this by leveraging our time-tested technology and tools in combination with matchless acumen and comprehensive data roadmap planning.
Every day, the MediQuant team converts, migrates, organizes and archives healthcare data for unparalleled reliability and performance.
Lower Expenses Up to 80%
Fortify Data Security and Compliance
Reduce Your IT Footprint
Retain Access to Active Data
Health Data Management Solutions
Data Conversion
Benefit from our decades of data management expertise.
Data Archiving
Learn why MediQuant is the safest and best choice.
Data Migration
Explore MediQuant’s proven methodology and tools.
Our Customers








































































































What Our Customers Say
MediQuant is a proven strategic partner in healthcare data management that drives smart decision-making, clinical excellence and strong financial performance.
Contact Us Today



